Netanya Sandler Utay of the University of Texas Medical Branch and Jintanat Ananworanich of the US Military HIV Research Program and colleagues in their abstract at CROI 2015 showed that Despite Early Antiretrovitral Treatment Inflammation and gut leakage remains elevated (Utay NS et al. Inflammation persists despite early initiation of ART in acute HIV infection. 2015 Conference on Retroviruses and Opportunistic Infections (CROI), Seattle, abstract 47, 2015)
Among the HIV-positive participants, the median CD4 T-cell count at study entry was 384 cells/mm3 (range 293-525) and the median HIV viral load was 5.6 log10 copies/ml. Using Ananworanich’s 4th generation staging system, 20 people were diagnosed during stage 1 of infection (HIV RNA positive; median 12 days after HIV acquisition), 15 during stage 2 (p24 antigen positive; median 16 days) and 43 during stage 3 (HIV antibody positive; median 18 days). About 40% started a standard ART regimen consisting of efavirenz (Sustiva) plus tenofovir/emtricitabine (the drugs in Truvada), while more than half started a more intensive regimen containing the same three drugs plus maraviroc (Celsentri/Selzentry) and raltegravir (Isentress).
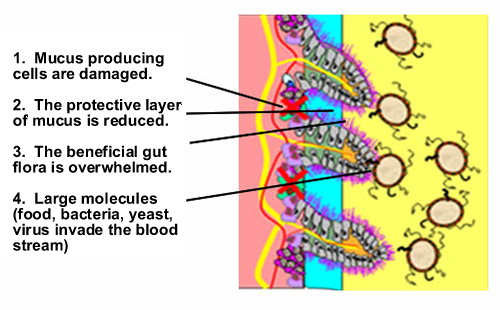
The researchers assessed changes in biomarkers of microbial translocation (damage to the gut that allows leakage of intestinal bacteria), inflammation, coagulation (blood clotting) and fibrosis (accumulation of connective tissue). These processes are associated with complications and death among people with chronic HIV infection, but how soon they occur and how they might be affected by early treatment is not well understood.
Utay and her team measured plasma levels of the following biomarkers at the time of HIV diagnosis or study entry (week 0) and again at weeks 2, 12, 24, 36, 48 and 96:
- Intestinal fatty acid binding protein (I-FABP), a marker of turnover of enterocytes, a type of absorptive cell in the gut lining;
- Hyaluronic acid, a fibrosis marker;
- D-dimer, a coagulation marker;
- C-reactive protein (CRP), an inflammation marker;
- Soluble CD14 (sCD14), an immune cell receptor that recognizes the bacterial toxin lipopolysaccharide (LPS) and is a marker for microbial translocation and monocyte activation;
- Interleukin 6 (IL-6), a pro-inflammatory cytokine;
- IL-6 receptor (IL-6R), a cytokine receptor that facilitates IL-6 signaling.
At week 0 all biomarker levels were significantly higher in HIV-positive participants — whether they were diagnosed at stage 1, 2 or 3 of acute infection — compared to the HIV-negative group, and they generally remained elevated through weeks 48 and 96. HIV-negative participants saw no changes in any of these biomarkers over the course of the study.
I-FABP — the marker of gut damage — increased significantly by week 2 in HIV-positive people at all stages of acute infection, and remained elevated after starting ART.
Hyaluronic acid levels were significantly elevated at all time points in the HIV-positive group. Levels tended to fluctuate — falling around week 2, rising around week 24, then falling again — but never fell to the level of the HIV-negative group.
D-dimer levels were significantly higher at weeks 0 and 2 in HIV-positive compared to HIV-negative people, but decreased by week 12 and reached levels similar to those of the uninfected group.
CRP levels in the HIV-positive group were elevated at week 0, then decreased from week 2 to week 12; however, levels remained significantly higher at all time points except week 48 compared to the HIV-negative group. sCD14 levels decreased by week 12, but nevertheless remained significantly elevated at all time points compared to the HIV-negative group.
IL-6 levels in HIV-positive people with all stages of acute infection showed a less consistent pattern, but generally decreased by week 24 or 48. Soluble IL-6R levels decreased significantly in the HIV-positive group by week 24 on ART.
“Biomarkers of enterocyte death, microbial translocation, inflammation, coagulation and fibrosis increase early in acute HIV infection,” the researchers concluded. “I-FABP increases and remains elevated during infection despite suppressive ART, suggesting on-going enterocyte damage or turnover.”
“Suppressive ART started during acute HIV infection does not eradicate the inflammation associated with increased morbidity and mortality in treated chronic HIV infection,” they continued. However, they noted, most biomarkers decrease in people who start ART during acute infection to levels lower than those observed in patients who start ART during chronic HIV infection.